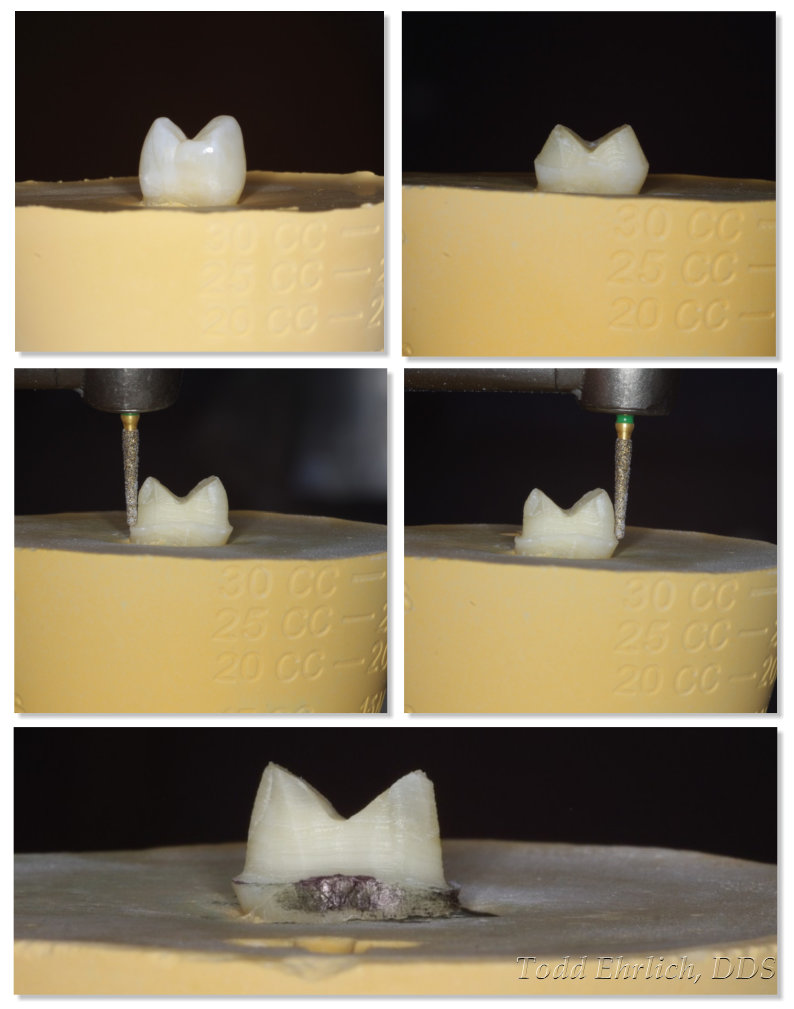
In all of the years of CAD/CAM dentistry, this discussion has always happened. “Over milling” is where the burs remove more material on the intaglio surface so that the restoration will seat without binding. The “over mill” is dependent on the prep surface, the thickness of the spacer, the bur geometry, and the angle for which the bur can mill. These variables can be dependent on each other.
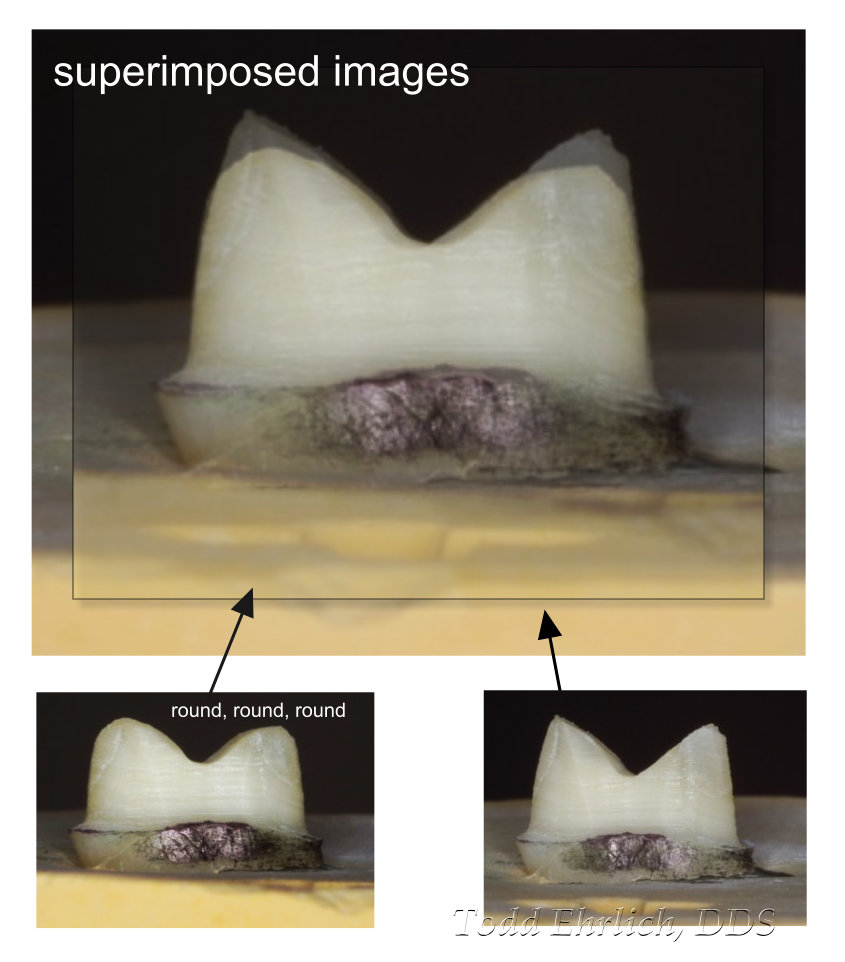
Round, round, round!
The main thing that the clinician can control is the preparation surface. Rounded transitions are the key to reducing over milling. If the rounded transition fits into the geometry of the bur milling the surface, you will have little to no over milling. Many years ago in the history of CEREC, there was ONLY a cylinder bur that was 1.6mm in diameter. Because of it’s large diameter, it tended to over mill a lot more than what we see today with our smaller diameter burs. Imagine the step bur that is in your milling unit while you are prepping the tooth. It is like a mirror image to your own handpiece if you were PREPPING the tooth completely vertical. Will your sharp transitions fit what the step bur could do in the mirrored image of your preparation? YOU are a multi-axis milling unit! The MCXL and other chairside milling units are limited to 4 axes! (I will discuss the pros/cons of 4 axis milling later.) But…. do NOT think that smaller equals better! Burs bend during grinding! This is compensated by the parameter in CEREC called “occlusal offset.” (I will discuss this in another article.) Do you think smaller burs bend more, or less, than larger diameter burs? Does the material “hardness” have an impact? Think about those things very hard before you just jump on to a smaller diameter bur bandwagon. 🙂

Less 4, More 6!
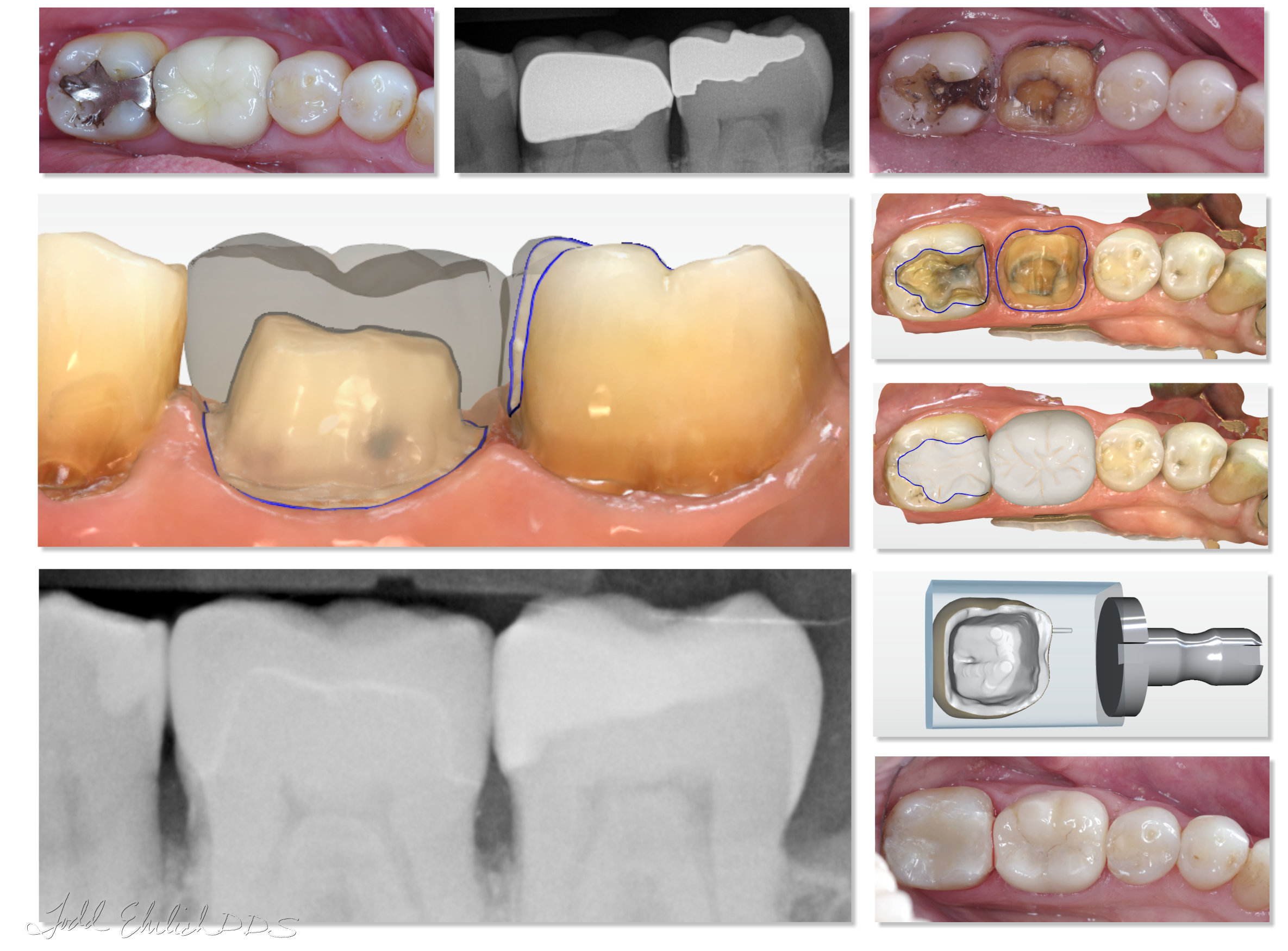
Dentists have been trained that “4-6 degree taper” is the holy grail of vertical walls. This may be true, but as clinicians we have a HUGE range of what we think is 4-6 degrees of taper! I know because I’ve watched hundreds of dentists prepare the same dentoform teeth! The limited 4-6 degree taper is for the draw of the restoration and control the resistance of lateral forces during function and the retention of the restoration in vertical vectors. As a clinician we can try to “error” on a more vertical preparation of the lateral walls so that the restoration will stay on. Makes us feel better. That is fine, but when the walls are vertical and you are using a 4-axis milling unit (CEREC and other chairside milling units) the bur that mills the intaglio surface may have to remove ceramic near the internal portion of the margin just to REACH to occlusal portions of the lateral wall – occlusal surface transition. In other words, it has to reach the areas to mill, but if we don’t give it “room” to get there, it’s going to take material away to do it. In our classes, I encourage dentists, “prep less 4, and more 6!” This is the visual that I want them to have because they are probably prepping more like 0 degrees, or maybe even undercutting. It is OK to taper the walls more for milled ceramics! The 4-6 degree taper holy grail was from when gold and porcelain-fused-to-metal were the only options for crowns. Why do we “feel” like it transitions into chairside cad/cam machined materials?
Spacer Wars
I was trained probably just like you: we want as little spacer as possible for a better intimate fit of the prosthesis to tooth. It was burned into my soul, and it is hard to think otherwise, but is it actually clinically significant? Again, this was started with metal restorations and limited cements like zinc phosphate. Our materials are highly improved in the last 30 years with ceramics, cements, and bonding. I am amused with statements that I see online about how small the clinician is making the spacer! It is like a competition with some! However, tighter spacer may only lead to a restoration that doesn’t seat completely, doesn’t comply with the viscosity of the cement, and enhances over milling. Why are we thinking this? I would surmise that it comes from how we were trained with stone models. The physical spacer application on a stone die is not nearly as accurate and predictable as our digitally designed spacers! You may have thought that your analog spacer was less than 100 microns for your PFM and gold prior to using CEREC! Then that magic number transitions into your digitally milled restorations, and you find out what 100 microns really is! 🙂 Plus, there are a lot of long-term retrospective studies showing the success of ceramic restorations with huge spacers. When you look at the spacer settings with those restorations, you would be amazed. Remember these studies were done 15+ years ago with limited milling units. I’ll encourage you to bump up your spacer 20 microns. You and your patient will live, and the restoration may just “fit” better!
Axis of Evil!
Our current technology of physically milling, or grinding, is limited in the motion range and angle of the motors. Keep this in mind: the more axes that are added, the more complexity added to software, motors, and manufacturing. More axes to the milling unit also adds more time and cost. There is a “sweet spot” for what your needs are, and it isn’t hard to figure out. A dental laboratory using CAD/CAM needs as many milling axes as they can get because they are making prosthetics for a wide range of clinical situations and materials. They also have the luxury of time. In general, it doesn’t matter if the crown takes 10 minutes or 30 minutes to mill. They are also milling a lot of them for many clients. Therefore, they will use bigger milling units and bigger pieces of material (pucks.) A dentist has different needs for machining: fast, predictable, and accurate, but limited in scope and “clients.” The limitation is basically fixed restorative dentistry: crowns, veneers, onlays, etc., for one or two doctors. Different worlds completely, with some overlap, of course. In my opinion, a fast 4 axis milling unit is better for my clinical needs than a slower 5 axis milling unit regardless of cost. This is with the caveat that the preparations are made appropriately!
Our online education platform is awesome! Hundreds of videos that help your day-to-day use of CEREC! Works directly through your Apple or Android devices!


