As great as dental x-rays are today with our high resolution digital sensors or the convenient phosphor plates, they come with MAJOR limitations. Dental x-rays (the typical bite-wings and periapicals) are pretty much the same as they’ve been for 50+ years. The improvements have obviously come in the realms of:
greatly reduced x-ray exposure
digital enhancement
faster technique
elimination of developing chemicals
easier data transfer
 But, even with all of these advancements, we are STILL looking at the many shades of grey! We are judging potential pathology on these shades! This isn’t much different than a clinician in the 1950’s holding up the x-ray over his head and evaluating through the overhead light! We just do the same thing by zooming in the resolution of the image on our computer monitors! The information is the same but just enhanced in our modern day digital x-ray technologies. This is relatively NOTHING new. Only improved.
But, even with all of these advancements, we are STILL looking at the many shades of grey! We are judging potential pathology on these shades! This isn’t much different than a clinician in the 1950’s holding up the x-ray over his head and evaluating through the overhead light! We just do the same thing by zooming in the resolution of the image on our computer monitors! The information is the same but just enhanced in our modern day digital x-ray technologies. This is relatively NOTHING new. Only improved.
Now, don’t get me wrong! X-rays are a vital aspect of the process to diagnose. They can show us an abscessed apex quickly and easily, but they ALSO leave a LOT to speculation, extrapolation, and estimation. This goes with the territory of any medical diagnosis! Experience, of course, matters. “Experience” is gained when the clinician sees enough examples of a particular situation that he/she can speculate what to do on subsequent similar situations. A major part of this dental experience comes from seeing many different types of dental materials exposed in the x-rays. Then, material types, and even brand variations of the materials, can have significantly different views on an x-ray image (for instance, “burnout” in 2D, or “beam hardening” in 3D.)
In general, metal-based restorative materials are very radio-opaque. Ok, we all know this: radio-opaque materials BLOCK OUT shades of grey. So a metal margin has the ability to completely block out recurrent caries, and clinically, it may be difficult visually to discern what exactly is going on under the restoration. We have to use our “experience” to give us clues for the best direction of treatment: monitor, repair, or restore.
There are the usual hard tissues to be seen in an x-ray: bone, enamel, dentin, etc. Sometimes soft tissue can be seen but it is nearly impossible to differentiate between types of soft tissue: gingiva, musculature, skin, etc. You throw in dental materials and there is even more to differentiate. Dental materials have a wide array of radio-opacity levels, i.e., multiple shades of grey.
If metal restorations were radiolucent or translucent how long would we really let them last?
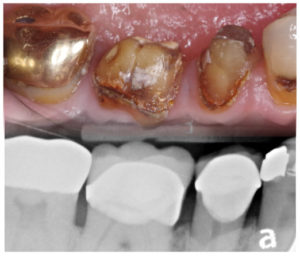 Just because a restoration is still in place and “functioning,” does it mean that there is no pathology? Could we be missing recurrent caries on exams because we can’t see under the restoration, and/or, the x-ray is blocked out by the metal? Of course! However, much of our dental culture is based on how long a material type LASTS rather than how well it services the patient as it is in the mouth. Should we let metal restorations last as long as we do? There are definitely 50 shades of grey on the answer to that!
Just because a restoration is still in place and “functioning,” does it mean that there is no pathology? Could we be missing recurrent caries on exams because we can’t see under the restoration, and/or, the x-ray is blocked out by the metal? Of course! However, much of our dental culture is based on how long a material type LASTS rather than how well it services the patient as it is in the mouth. Should we let metal restorations last as long as we do? There are definitely 50 shades of grey on the answer to that!
In this case, there is not a lot, or any, evidence of recurrent caries on the x-rays of this quadrant. But if there is a large carious lesion at the buccal of the premolar, and maybe a question of visible integrity of the margins, it could be “assumed” there may be something going on at the margins of the crowns next to it. It really isn’t known until they are taken off!
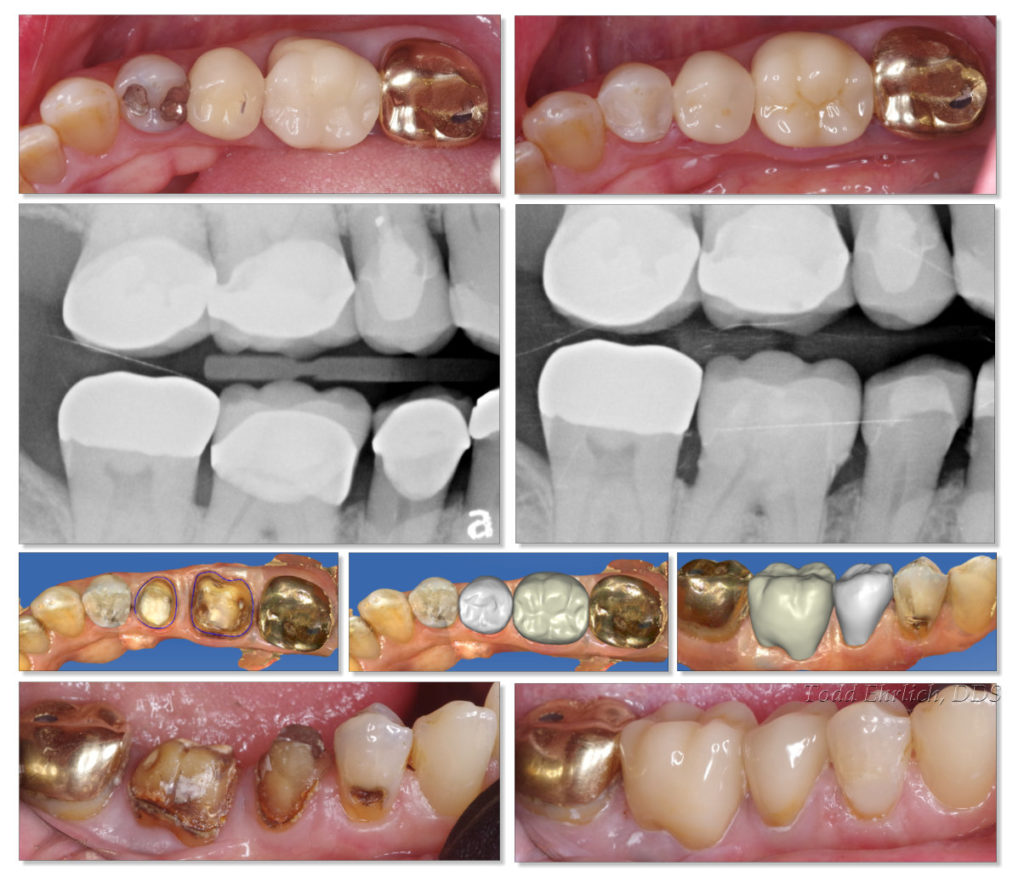 The PFM’s were removed and the extensive recurrent caries was very obvious. IF the radio-opaque PFM’s were actually translucent, how much sooner would the crowns been replaced or repaired? A year ago? Two years ago? 5 years ago? What would be the next stage for these teeth had they not been restored because there was no radiographic evidence?
The PFM’s were removed and the extensive recurrent caries was very obvious. IF the radio-opaque PFM’s were actually translucent, how much sooner would the crowns been replaced or repaired? A year ago? Two years ago? 5 years ago? What would be the next stage for these teeth had they not been restored because there was no radiographic evidence?
The very nature of visually opaque and radiographically radio-opaque makes it extremely difficult to diagnose recurrent caries without “experience.” The gold crown at #31 will also be replaced in the near future.
The next diagnostic chapter after x-rays will be revolutionary.
Our online education platform is awesome! Hundreds of videos that help your day-to-day use of CEREC! Works directly through your Apple or Android devices!


